Dry EyeDry eye is a condition in which there are insufficient tears to lubricate and nourish the eye. Tears are necessary for maintaining the health of the front surface of the eye and for providing clear vision. People with dry eyes either do not produce enough tears or have a poor quality of tears. Dry eye is a common and often chronic problem, particularly in older adults.
With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter in the eye, and keep the surface of the eyes smooth and clear. Excess tears in the eyes flow into small drainage ducts, in the inner corners of the eyelids, which drain in the back of the nose.
Dry eyes can result from an improper balance of tear production and drainage.
People with dry eyes may experience symptoms of irritated, gritty, scratchy, or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eyes may damage the front surface of the eye and impair vision.
Treatments for dry eyes aim to restore or maintain the normal amount of tears in the eye to minimize dryness and related discomfort and to maintain eye health.
What causes dry eyes?
The majority of people over the age of 65 experience some symptoms of dry eyes.The development of dry eyes can have many causes. They include:
How are dry eyes diagnosed?
Dry eyes can be diagnosed through a comprehensive eye examination. Testing, with special emphasis on the evaluation of the quantity and quality of tears produced by the eyes, may include:
[back to top]
How are dry eyes treated?
One of the primary approaches used to manage and treat mild cases of dry eyes is adding tears using over-the-counter artificial tear solutions.Dry eyes can be a chronic condition, but your optometrist can prescribe treatment to keep your eyes healthy, more comfortable, and prevent your vision from being affected. The primary approaches used to manage and treat dry eyes include adding tears, conserving tears, increasing tear production, and treating the inflammation of the eyelids or eye surface that contributes to the dry eyes.
Information is from the American Optometric Association website.
For more information visit mydryeyes.com
With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter in the eye, and keep the surface of the eyes smooth and clear. Excess tears in the eyes flow into small drainage ducts, in the inner corners of the eyelids, which drain in the back of the nose.
Dry eyes can result from an improper balance of tear production and drainage.
- Inadequate amount of tears – Tears are produced by several glands in and around the eyelids. Tear production tends to diminish with age, with various medical conditions, or as a side effect of certain medicines. Environmental conditions such as wind and dry climates can also affect tear volume by increasing tear evaporation. When the normal amount of tear production decreases or tears evaporate too quickly from the eyes, symptoms of dry eye can develop.
- Poor quality of tears – Tears are made up of three layers: oil, water, and mucus. Each component serves a function in protecting and nourishing the front surface of the eye. A smooth oil layer helps to prevent evaporation of the water layer, while the mucin layer functions in spreading the tears evenly over the surface of the eye. If the tears evaporate too quickly or do not spread evenly over the cornea due to deficiencies with any of the three tear layers, dry eye symptoms can develop.
People with dry eyes may experience symptoms of irritated, gritty, scratchy, or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eyes may damage the front surface of the eye and impair vision.
Treatments for dry eyes aim to restore or maintain the normal amount of tears in the eye to minimize dryness and related discomfort and to maintain eye health.
What causes dry eyes?
The majority of people over the age of 65 experience some symptoms of dry eyes.The development of dry eyes can have many causes. They include:
- Age – dry eye is a part of the natural aging process. The majority of people over age 65 experience some symptoms of dry eyes.
- Gender – women are more likely to develop dry eyes due to hormonal changes caused by pregnancy, the use of oral contraceptives, and menopause.
- Medications – certain medicines, including antihistamines, decongestants, blood pressure medications and antidepressants, can reduce the amount of tears produced in the eyes.
- Medical conditions – persons with rheumatoid arthritis, diabetes and thyroid problems are more likely to have symptoms of dry eyes. Also, problems with inflammation of the eyelids (blepharitis), inflammation of the surfaces of the eye, or the inward or outward turning of eyelids can cause dry eyes to develop.
- Environmental conditions – exposure to smoke, wind and dry climates can increase tear evaporation resulting in dry eye symptoms. Failure to blink regularly, such as when staring at a computer screen for long periods of time, can also contribute to drying of the eyes.
- Other factors – long term use of contact lenses can be a factor in the development of dry eyes. Refractive eye surgeries, such as LASIK, can cause decreased tear production and dry eyes.
How are dry eyes diagnosed?
Dry eyes can be diagnosed through a comprehensive eye examination. Testing, with special emphasis on the evaluation of the quantity and quality of tears produced by the eyes, may include:
- Patient history to determine any symptoms the patient is experiencing and the presence of any general health problems, medications taken, or environmental factors that may be contributing to the dry eye problem.
- External examination of the eye, including lid structure and blink dynamics.
- Evaluation of the eyelids and cornea using bright light and magnification.
- Measurement of the quantity and quality of tears for any abnormalities. Special dyes may be instilled in the eyes to better observe tear flow and to highlight any changes to the outer surface of the eye caused by insufficient tears.
[back to top]
How are dry eyes treated?
One of the primary approaches used to manage and treat mild cases of dry eyes is adding tears using over-the-counter artificial tear solutions.Dry eyes can be a chronic condition, but your optometrist can prescribe treatment to keep your eyes healthy, more comfortable, and prevent your vision from being affected. The primary approaches used to manage and treat dry eyes include adding tears, conserving tears, increasing tear production, and treating the inflammation of the eyelids or eye surface that contributes to the dry eyes.
- Adding tears – Mild cases of dry eyes can often be managed using over-the-counter artificial tear solutions. These can be used as often as needed to supplement natural tear production. Preservative-free artificial tear solutions are recommended because they contain fewer additives that could further irritate the eyes. However, some people may have persistent dry eyes that don’t respond to artificial tears alone. Additional steps need to be taken to treat their dry eyes.
- Conserving tears – An additional approach to reducing the symptoms of dry eyes is to keep natural tears in the eyes longer. This can be done by blocking the tear ducts through which the tears normally drain. The tear ducts can be blocked with tiny silicone or gel-like plugs that can be removed, if needed. A surgical procedure to permanently close tear ducts can also be used. In either case, the goal is to keep the available tears in the eye longer to reduce problems related to dry eyes.
- Increasing tear production – Prescription eye drops that help to increase production of tears can be recommended by your optometrist, as well as omega-3 fatty acid nutritional supplements.
- Treatment of the contributing eyelid or ocular surface inflammation – Prescription eye drops or ointments, warm compresses and lid massage, or eyelid cleaners may be recommended to help decrease inflammation around the surface of the eyes.
- Remembering to blink regularly when reading or staring at a computer screen for long periods of time.
- Increasing the level of humidity in the air at work and at home.
- Wearing sunglasses outdoors, particularly those with wrap around frame design, to reduce exposure to drying winds and sun.
- Using nutritional supplements containing essential fatty acids may help decrease dry eye symptoms in some people. Ask your optometrist if the use of dietary supplements could be of help for your dry eye problems.
Information is from the American Optometric Association website.
For more information visit mydryeyes.com
Cataracts
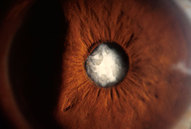
A cataract is a cloudy or opaque area in the normally clear
lens of the eye. Depending upon its size and location, it can interfere with
normal vision. Most cataracts develop in people over age 55, but they
occasionally occur in infants and young children. Usually cataracts develop in both eyes, but one may be worse than the other. Researchers have linked eye-friendly nutrients such as lutein/zeaxanthin, vitamin C, vitamin E, and zinc to reducing the risk of certain eye diseases, including cataracts. For more information on the importance of good nutrition and eye health, please see the eye nutrition section.
The lens is located inside the eye behind the iris, the colored part of the
eye. The lens focuses light on the back of the eye, the retina. The lens is made
of mostly proteins and water. Clouding of the lens occurs due to changes in the
proteins and lens fibers.
The lens is composed of layers like an onion. The outermost is the capsule.
The layer inside the capsule is the cortex, and the innermost layer is the
nucleus. A cataract may develop in any of these areas and is described based on
its location in the lens:
lens of the eye. Depending upon its size and location, it can interfere with
normal vision. Most cataracts develop in people over age 55, but they
occasionally occur in infants and young children. Usually cataracts develop in both eyes, but one may be worse than the other. Researchers have linked eye-friendly nutrients such as lutein/zeaxanthin, vitamin C, vitamin E, and zinc to reducing the risk of certain eye diseases, including cataracts. For more information on the importance of good nutrition and eye health, please see the eye nutrition section.
The lens is located inside the eye behind the iris, the colored part of the
eye. The lens focuses light on the back of the eye, the retina. The lens is made
of mostly proteins and water. Clouding of the lens occurs due to changes in the
proteins and lens fibers.
The lens is composed of layers like an onion. The outermost is the capsule.
The layer inside the capsule is the cortex, and the innermost layer is the
nucleus. A cataract may develop in any of these areas and is described based on
its location in the lens:
- A nuclear cataract is located in the center of the lens.
The nucleus tends to darken changing from clear to yellow and sometimes brown. - A cortical cataract affects the layer of the lens
surrounding the nucleus. It is identified by its unique wedge or spoke
appearance. - A posterior capsular cataract is found in the back outer
layer of the lens. This type often develops more rapidly.
glaucoma
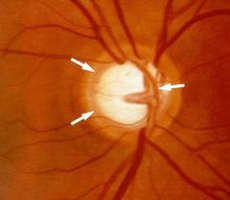
The most common form of glaucoma, primary open-angle glaucoma, is associated with an increase in the fluid pressure inside the eye. This increase in pressure may cause progressive damage to the optic nerve and loss of nerve fibers. Vision loss may result. Advanced glaucoma may even cause blindness. Not everyone with high eye pressure will develop glaucoma, and many people with normal eye pressure will develop glaucoma. When the pressure inside an eye is too high for that particular optic nerve, whatever that pressure measurement may be, glaucoma will develop. Primary open-angle glaucoma develops slowly and usually without any symptoms. Many people do not become aware they have the condition until significant vision loss has occurred. It initially affects peripheral or side vision, but can advance to central vision loss. If left untreated, glaucoma can lead to significant loss of vision in both eyes, and may even lead to blindness.
A less common type of glaucoma, acute angle closure glaucoma, usually occurs abruptly due to a rapid increase of pressure in the eye. Its symptoms may include severe eye pain, nausea, redness in the eye, seeing colored rings around lights, and blurred vision. This condition is an ocular emergency, and medical attention should be sought immediately, as severe vision loss can occur quickly.
Glaucoma cannot currently be prevented, but if diagnosed and treated early it can usually be controlled. Medication or surgery can slow or prevent further vision loss. However, vision already lost to glaucoma cannot be restored. That is why the American Optometric Association recommends an annual dilated eye
examination for people at risk for glaucoma as a preventive eye care measure. Depending on your specific condition, your doctor may recommend more frequent examinations.
Certain factors can increase the risk for developing glaucoma. They include:
A less common type of glaucoma, acute angle closure glaucoma, usually occurs abruptly due to a rapid increase of pressure in the eye. Its symptoms may include severe eye pain, nausea, redness in the eye, seeing colored rings around lights, and blurred vision. This condition is an ocular emergency, and medical attention should be sought immediately, as severe vision loss can occur quickly.
Glaucoma cannot currently be prevented, but if diagnosed and treated early it can usually be controlled. Medication or surgery can slow or prevent further vision loss. However, vision already lost to glaucoma cannot be restored. That is why the American Optometric Association recommends an annual dilated eye
examination for people at risk for glaucoma as a preventive eye care measure. Depending on your specific condition, your doctor may recommend more frequent examinations.
Certain factors can increase the risk for developing glaucoma. They include:
- Age – People over age 60 are at increased risk for the disease. For African Americans, however, the increase in risk begins after age 40. The risk of developing glaucoma increases slightly with each year of age.
- Race – African Americans are significantly more likely to get glaucoma than are Caucasians, and they are much more likely to suffer permanent vision loss as a result. People of Asian descent are at higher risk of angle-closure glaucoma and those of Japanese descent are more prone to low-tension glaucoma.
- Family history of glaucoma – Having a family history of glaucoma increases the risk of developing glaucoma.
- Medical conditions – Some studies indicate that diabetes may increases the risk of developing glaucoma, as do high blood pressure and heart disease.
- Physical injuries to the eye – Severe trauma, such as being hit in the eye, can result in immediate increased eye pressure and future increases in pressure due to internal damage. Injury can also dislocate the lens, closing the drainage angle, and increasing pressure.
- Other eye-related risk factors – Eye anatomy, namely corneal thickness and optic nerve appearance indicate risk for development of glaucoma. Conditions such as retinal detachment, eye tumors, and eye
inflammations may also induce glaucoma. Some studies suggest that high amounts of nearsightedness may also be a risk factor for the development of glaucoma. - Corticosteroid use – Using corticosteroids for prolonged periods of time appears to put some people at risk of getting secondary glaucoma.
diabetic retinopathy
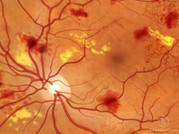
Diabetic retinopathy is a condition occurring in persons with diabetes, which causes progressive damage to the retina, the light sensitive lining at the back of the eye. It is a serious sight-threatening complication of diabetes.
Diabetes is a disease that interferes with the body's ability to use and
store sugar, which can cause many health problems. Too much sugar in the blood can cause damage throughout the body, including the eyes. Over time, diabetes affects the circulatory system of the retina.
Diabetic retinopathy is the result of damage to the tiny blood vessels that nourish the retina. They leak blood and other fluids that cause swelling of retinal tissue and clouding of vision. The condition usually affects both eyes. The longer a person has diabetes, the more likely they will develop diabetic retinopathy. If left untreated, diabetic retinopathy can cause blindness.
Symptoms of diabetic retinopathy include: seeing spots or floaters in your field of vision, blurred vision, having a dark or empty spot in the center of your vision, and difficulty seeing well at night.
In patients with diabetes, prolonged periods of high blood sugar can lead to the accumulation of fluid in the lens inside the eye that controls eye focusing. This changes the curvature of the lens and results in the development of symptoms of blurred vision. The blurring of distance vision as a result of lens swelling will subside once the blood sugar levels are brought under control. Better control of blood sugar levels in patients with diabetes also slows the onset and progression of diabetic retinopathy.
Often there are no visual symptoms in the early stages of diabetic retinopathy. That is why the American Optometric Association recommends that everyone with diabetes have a comprehensive dilated eye examination once a year. Early detection and treatment can limit the potential for significant vision loss from diabetic retinopathy.
Treatment of diabetic retinopathy varies depending on the extent of the disease. It may require laser surgery to seal leaking blood vessels or to discourage new leaky blood vessels from forming. Injections of medications into the eye may be needed to decrease inflammation or stop the formation of new blood vessels. In more advanced cases, a surgical procedure to remove and replace the gel-like fluid in the back of the eye, called the vitreous, may be needed. A retinal detachment, defined as a separation of the light-receiving lining in the back of the eye, resulting from diabetic retinopathy, may also require surgical repair.
If you are a diabetic, you can help prevent or slow the development of diabetic retinopathy by taking your prescribed medication, sticking to your diet, exercising regularly, controlling high blood pressure and avoiding alcohol and smoking.
Diabetes is a disease that interferes with the body's ability to use and
store sugar, which can cause many health problems. Too much sugar in the blood can cause damage throughout the body, including the eyes. Over time, diabetes affects the circulatory system of the retina.
Diabetic retinopathy is the result of damage to the tiny blood vessels that nourish the retina. They leak blood and other fluids that cause swelling of retinal tissue and clouding of vision. The condition usually affects both eyes. The longer a person has diabetes, the more likely they will develop diabetic retinopathy. If left untreated, diabetic retinopathy can cause blindness.
Symptoms of diabetic retinopathy include: seeing spots or floaters in your field of vision, blurred vision, having a dark or empty spot in the center of your vision, and difficulty seeing well at night.
In patients with diabetes, prolonged periods of high blood sugar can lead to the accumulation of fluid in the lens inside the eye that controls eye focusing. This changes the curvature of the lens and results in the development of symptoms of blurred vision. The blurring of distance vision as a result of lens swelling will subside once the blood sugar levels are brought under control. Better control of blood sugar levels in patients with diabetes also slows the onset and progression of diabetic retinopathy.
Often there are no visual symptoms in the early stages of diabetic retinopathy. That is why the American Optometric Association recommends that everyone with diabetes have a comprehensive dilated eye examination once a year. Early detection and treatment can limit the potential for significant vision loss from diabetic retinopathy.
Treatment of diabetic retinopathy varies depending on the extent of the disease. It may require laser surgery to seal leaking blood vessels or to discourage new leaky blood vessels from forming. Injections of medications into the eye may be needed to decrease inflammation or stop the formation of new blood vessels. In more advanced cases, a surgical procedure to remove and replace the gel-like fluid in the back of the eye, called the vitreous, may be needed. A retinal detachment, defined as a separation of the light-receiving lining in the back of the eye, resulting from diabetic retinopathy, may also require surgical repair.
If you are a diabetic, you can help prevent or slow the development of diabetic retinopathy by taking your prescribed medication, sticking to your diet, exercising regularly, controlling high blood pressure and avoiding alcohol and smoking.
macular degeneration
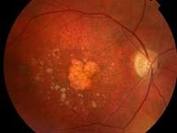
Age-Related Macular Degeneration (AMD) is the leading cause of severe vision loss in adults over age 50. The Centers for Disease Control and Prevention estimate that 1.8 million people have AMD and another 7.3 million are at substantial risk for vision loss from AMD. Caucasians are at higher risk for developing AMD than other races. Women also develop AMD at an earlier age than men. This eye disease occurs when there are changes to the macula, a small portion of the retina that is located on the inside back layer of the eye. AMD is a loss of central vision that can occur in two forms: “dry” or atrophic and “wet” or exudative.
Most people with macular degeneration have the dry form, for which there is no known treatment. The less common wet form may respond to laser procedures, if diagnosed and treated early.
Some common symptoms are: a gradual loss of ability to see objects clearly, distorted vision, a gradual loss of color vision, and a dark or empty area appearing in the center of vision. If you experience any of these, contact your doctor of optometryimmediately for a comprehensive examination. Central vision that is lost to macular degeneration cannot be restored. However, low vision devices, such as telescopic and microscopic lenses, can be prescribed to maximize existing vision.
Researchers have linked eye-friendly nutrients such as lutein/zeaxanthin, vitamin C, vitamin E, and zinc to reducing the risk of certain eye diseases, including macular degeneration.
Most people with macular degeneration have the dry form, for which there is no known treatment. The less common wet form may respond to laser procedures, if diagnosed and treated early.
Some common symptoms are: a gradual loss of ability to see objects clearly, distorted vision, a gradual loss of color vision, and a dark or empty area appearing in the center of vision. If you experience any of these, contact your doctor of optometryimmediately for a comprehensive examination. Central vision that is lost to macular degeneration cannot be restored. However, low vision devices, such as telescopic and microscopic lenses, can be prescribed to maximize existing vision.
Researchers have linked eye-friendly nutrients such as lutein/zeaxanthin, vitamin C, vitamin E, and zinc to reducing the risk of certain eye diseases, including macular degeneration.
dry eye
Dry eye is a condition in which there are insufficient tears to lubricate and nourish the eye. Tears are necessary for maintaining the health of the front surface of the eye and for providing clear vision. People with dry eyes either do not produce enough tears or have a poor quality of tears. Dry eye is a common and often chronic problem, particularly in older adults.
With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter in the eye, and keep the surface of the eyes smooth and clear. Excess tears in the eyes flow into small drainage ducts, in the inner corners of the eyelids, which drain in the back of the nose.
Dry eyes can result from an improper balance of tear production and drainage.The most common form of dry eyes is due to an inadequate amount of the water layer of tears. This condition, called keratoconjunctivitis sicca (KCS), is also referred to as dry eye syndrome.
People with dry eyes may experience symptoms of irritated, gritty, scratchy, or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eyes may damage the front surface of the eye and impair vision.
Treatments for dry eyes aim to restore or maintain the normal amount of tears in the eye to minimize dryness and related discomfort and to maintain eye health.
With each blink of the eyelids, tears are spread across the front surface of the eye, known as the cornea. Tears provide lubrication, reduce the risk of eye infection, wash away foreign matter in the eye, and keep the surface of the eyes smooth and clear. Excess tears in the eyes flow into small drainage ducts, in the inner corners of the eyelids, which drain in the back of the nose.
Dry eyes can result from an improper balance of tear production and drainage.The most common form of dry eyes is due to an inadequate amount of the water layer of tears. This condition, called keratoconjunctivitis sicca (KCS), is also referred to as dry eye syndrome.
People with dry eyes may experience symptoms of irritated, gritty, scratchy, or burning eyes, a feeling of something in their eyes, excess watering, and blurred vision. Advanced dry eyes may damage the front surface of the eye and impair vision.
Treatments for dry eyes aim to restore or maintain the normal amount of tears in the eye to minimize dryness and related discomfort and to maintain eye health.
Amblyopia
Lazy eye, or amblyopia, is the loss or lack of development
of central vision in one eye that is unrelated to any eye health problem and is
not correctable with lenses. It can result from a failure to use both eyes
together. Lazy eye is often associated with crossed-eyes or a large difference
in the degree of nearsightedness or farsightedness between the two eyes. It
usually develops before the age of 6, and it does not affect side vision.
Symptoms may include noticeably favoring one eye or a tendency to bump into
objects on one side. Symptoms are not always obvious.
Treatment for lazy eye may include a combination of prescription lenses,
prisms, vision therapy and eye patching. Vision therapy teaches the two eyes how
to work together, which helps prevent lazy eye from reoccurring.
Early diagnosis increases the chance for a complete recovery. This is one
reason why the American Optometric Association recommends that children have a
comprehensive optometric examination by the age of 6 months and again at age 3.
Lazy eye will not go away on its own. If not diagnosed until the pre-teen, teen
or adult years, treatment takes longer and is often less effective.
of central vision in one eye that is unrelated to any eye health problem and is
not correctable with lenses. It can result from a failure to use both eyes
together. Lazy eye is often associated with crossed-eyes or a large difference
in the degree of nearsightedness or farsightedness between the two eyes. It
usually develops before the age of 6, and it does not affect side vision.
Symptoms may include noticeably favoring one eye or a tendency to bump into
objects on one side. Symptoms are not always obvious.
Treatment for lazy eye may include a combination of prescription lenses,
prisms, vision therapy and eye patching. Vision therapy teaches the two eyes how
to work together, which helps prevent lazy eye from reoccurring.
Early diagnosis increases the chance for a complete recovery. This is one
reason why the American Optometric Association recommends that children have a
comprehensive optometric examination by the age of 6 months and again at age 3.
Lazy eye will not go away on its own. If not diagnosed until the pre-teen, teen
or adult years, treatment takes longer and is often less effective.
Myopia
Nearsightedness, or myopia, as it is medically termed, is a vision condition
in which close objects are seen clearly, but objects farther away appear
blurred. Nearsightedness occurs if the eyeball is too long or the cornea, the
clear front cover of the eye, has too much curvature. As a result, the light
entering the eye isn’t focused correctly and distant objects look blurred.
Nearsightedness is a very common vision condition affecting nearly 30 percent
of the U.S. population. Some research supports the theory that nearsightedness
is hereditary. There is also growing evidence that it is influenced by the
visual stress of too much close work.
Generally, nearsightedness first occurs in school-age children. Because the
eye continues to grow during childhood, it typically progresses until about age
20. However, nearsightedness may also develop in adults due to visual stress or
health conditions such as diabetes.
A common sign of nearsightedness is difficulty with the clarity of distant
objects like a movie or TV screen or the chalkboard in school. A comprehensive optometric exam will include testing for nearsightedness. An optometrist can prescribe eyeglasses or contact
lenses that correct nearsightedness by bending the visual images that enter the
eyes, focusing the images correctly at the back of the eye. Depending on the
amount of nearsightedness, you may only need to wear glasses or contact lenses
for certain activities, like watching a movie or driving a car. Or, if you are
very nearsighted, they may need to be worn all the time.
in which close objects are seen clearly, but objects farther away appear
blurred. Nearsightedness occurs if the eyeball is too long or the cornea, the
clear front cover of the eye, has too much curvature. As a result, the light
entering the eye isn’t focused correctly and distant objects look blurred.
Nearsightedness is a very common vision condition affecting nearly 30 percent
of the U.S. population. Some research supports the theory that nearsightedness
is hereditary. There is also growing evidence that it is influenced by the
visual stress of too much close work.
Generally, nearsightedness first occurs in school-age children. Because the
eye continues to grow during childhood, it typically progresses until about age
20. However, nearsightedness may also develop in adults due to visual stress or
health conditions such as diabetes.
A common sign of nearsightedness is difficulty with the clarity of distant
objects like a movie or TV screen or the chalkboard in school. A comprehensive optometric exam will include testing for nearsightedness. An optometrist can prescribe eyeglasses or contact
lenses that correct nearsightedness by bending the visual images that enter the
eyes, focusing the images correctly at the back of the eye. Depending on the
amount of nearsightedness, you may only need to wear glasses or contact lenses
for certain activities, like watching a movie or driving a car. Or, if you are
very nearsighted, they may need to be worn all the time.